
Announcement
(I) Benefit changes to Enhanced IncomeShield (EIS)
i) <REVISED> Pregnancy and Delivery-related Complications Benefit
From 1 April 2026, upon renewal of an EIS policy, we will now be covering all 30 conditions under Pregnancy and Delivery-related Complications benefit, with the flexibility to seek treatment from any registered medical practitioner.
Please refer to the policy conditions for further details.
(II) Launch of Optima Care rider and Essential Care rider
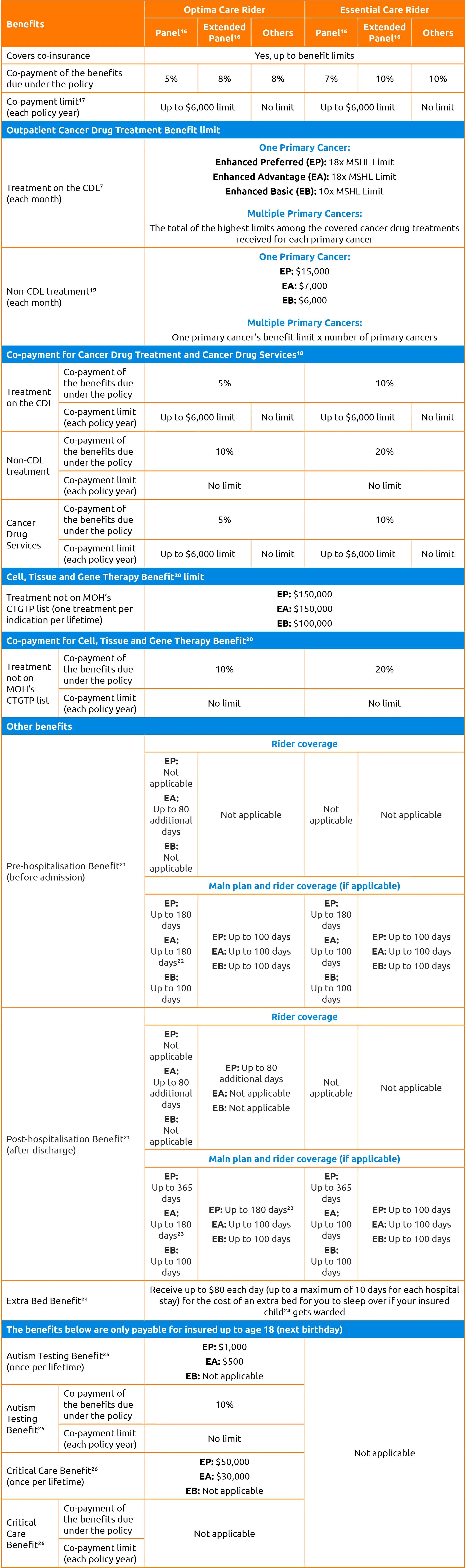
We have launched two new Integrated Shield Plan (IP) riders – Optima Care rider and Essential Care rider on 1 April 2026. The new IP riders, which are on average 32% cheaper than existing riders, feature a tiered co-payment model that is based on whether the treatment is provided by our panel, extended panel or others. The co-payment limit of up to $6,000 each policy year applies if the treatment is provided by our panel and extended panel. These riders are aligned to MOH’s new requirements for IP riders.
To offer our customers more protection against cancer, the Optima Care rider and Essential Care rider provide Cancer Drug Treatment Benefit, and Cell, Tissue and Gene Therapy Benefit (CTGTP) that covers treatment that is not on MOH’s CTGTP list. Other value-added benefits that also come with Optima Care rider include the Autism Testing Benefit and Critical Care Benefit, for insured up to age 18 (next birthday).
(III) Updates on Deluxe Care, Plus, Classic Care and Assist rider
As Deluxe Care rider and Classic Care rider do not meet MOH’s new requirements for IP riders, both riders will be withdrawn from 1 April 2026 onwards.
Policyholders will not be allowed to purchase the Deluxe Care rider or Classic Care rider from 1 April 2026. Existing policyholders of Deluxe Care rider will not be allowed to downgrade their rider to Classic Care rider, and those on Classic Care rider will not be allowed to upgrade to Deluxe Care rider.
If policyholders had bought a Deluxe Care, Plus, Classic Care or Assist rider before 27 November 2025, MOH’s new requirements for IP riders will not apply to the existing rider for now. At this juncture, the existing rider will continue to cover the IP main plan’s deductible and the co-payment limit remains at $3,000 in each policy year.
If the purchase of the Deluxe Care or Classic Care rider is between 27 November 2025 and 31 March 2026 (both dates inclusive), MOH’s new requirements for IP riders will apply to the Deluxe Care or Classic Care rider no later than the next policy renewal after 1 April 2028. More information will be shared with these policyholders in due course.
As part of our regular review of our IP plans and IP riders, we will continue to assess if changes will be needed to keep healthcare insurance sustainable for our policyholders. Like always, we will keep our policyholders informed of policy changes, if any.
(IV) Welcome discount for Enhanced IncomeShield, Optima Care rider and Essential Care rider (for new applications only)
Welcome Discount is a one-time 15% discount on the first-year premium for new policy applications – between 1 April 2026 and 31 March 2027 (both dates inclusive) – for Enhanced Preferred, Enhanced Advantage, Enhanced Basic, Optima Care rider and Essential Care rider, if there is no additional exclusions or premium loading applied to the policy upon policy issuance.
The Welcome Discount will be applied to the premium payable for the additional private insurance coverage portion of the main plans as well as the entire premium of eligible riders, provided that they are taken up together with a main plan. The Welcome Discount does not apply to the MediShield Life (MSHL) portion of the main plan. Other promotion terms and conditions apply.
Click here for the full Welcome Discount terms and conditions.
For more information on the changes, please read our FAQs here.
The Ministry of Health (MOH) has introduced new design requirements for Integrated Shield Plan (IP) riders that are made available for sale from 1 April 2026 onwards, as per their announcement on 26 November 2025.
The new requirements are:
i) No coverage for minimum IP deductible – IP riders will not cover the main plan’s minimum deductible.
ii) Higher co-payment cap – the minimum co-payment cap of IP riders will increase from $3,000 to $6,000 in each policy year.
The co-payment cap will also exclude the IP main plan’s minimum deductible.
For more details on the new requirements for IP riders, you can refer to MOH’s announcement at go.gov.sg/ipriderchanges2025.
For new customers
If you were to buy a Deluxe Care or Classic Care rider from 27 November 2025 to 31 March 2026 (both dates inclusive), the new requirements will apply to your Deluxe Care or Classic Care rider no later than your next policy renewal after 1 April 2028.
For existing customers
If you had bought a Deluxe Care, Plus, Classic Care or Assist rider before 27 November 2025, the new requirements will not apply to your existing rider for now. As part of our regular review of our IP plans and IP riders, we will continue to assess if changes will be needed to keep healthcare insurance sustainable for our policyholders. Like always, we will keep our policyholders informed of policy changes, if any.
For more details on the impact of the new requirements to Income’s IP riders, please read our FAQs here.
Should you have further queries, we would be most happy to assist you via your preferred mode of contact at income.com.sg/contact-us.
(I) Benefit changes to Enhanced IncomeShield (EIS)
Our IncomeShield health insurance plans are designed to provide policyholders with sustainable protection that meets their long-term healthcare needs. To do this, we annually review our scope of coverage to ensure that it keeps pace with the needs of our policyholders and medical advancements, and adjust premiums based on our claims experience for the year. As such, we would like to highlight the following changes that will take effect from 1 October 2025, upon renewal of the policy.
| Benefit changes | Enhanced IncomeShield | |||
| Enhanced Preferred | Enhanced Advantage | Enhanced Basic | Enhanced C | |
| Revised inpatient benefits | ✓ | ✓ | ✓ | ✓ |
| New outpatient benefits | ✓ | ✓ | ||
| Revised cell, tissue and gene therapy benefit | ✓ | ✓ | ✓ | ✓ |
| Revised pro-ration factors | ✓ | ✓ | ||
| Increased policy year limit | ✓ | |||
For more information on the changes, please read our FAQs here.
(II) Welcome discount for Enhanced IncomeShield, Deluxe Care rider and Classic Care rider (for new applications only)
A one-time 20% Welcome Discount will be applicable to the first-year premium for new applications – between 1 October 2025 and 30 September 2026 – for Enhanced Preferred, Enhanced Advantage, Enhanced Basic, Deluxe Care rider and Classic Care rider, if there is no additional exclusions or premium loading applied to the policy upon policy issuance.
The Welcome Discount will be applied to the premium payable for additional private insurance coverage portion (does not include the MediShield Life (MSHL) portion) of the main plans as well as the entire premium for any riders, provided it is taken up together with a main plan.
Click here for the full Welcome Discount terms and conditions.
Enjoy high levels of cancer coverage^
Hospitalisation can often feel overwhelming and frightening, not just because of the illness but also due to the fear of the high cost associated with hospital stays and treatments, especially via private hospital care. With Enhanced IncomeShield, you can enjoy high levels of cancer coverage^. Now, private hospital care is a lot less scary.
Did you know
Enjoy high levels of coverage with these benefits
Get up to 23x[6] MSHL monthly claim limit for outpatient treatments[7] listed on the Cancer Drug List (CDL) for one primary cancer.
Up to $250,000 for Cell, Tissue and Gene Therapy (CTGTP) listed on Ministry of Health’s (MOH) CTGTP list for one treatment per indication per lifetime[8,9], up to $150,000 for CTGTP treatments not listed on MOH’s CTGTP list for one treatment per indication per lifetime[20], and up to $100,000 for Proton Beam Therapy[8,10] for each policy year.
Covers up to $20,000[4] for each policy year.
Enjoy a one-time Autism Testing Benefit[25,27] reimbursement of up to $1,000 with a 10% co-payment if the insured child undergoes an autism test.
Enhance your MediShield Life coverage with Enhanced IncomeShield
Up to $1.5 million limit in each policy year[4] for medical treatment.
Coverage with no lifetime limit[5], so your loved ones are relieved of the financial burden if something unforeseen happens.
Reimbursement for all benefits, including pre- and post-hospitalisation coverage for up to 180 days and 365 days, respectively[11].
As charged coverage for selected benefits[12] for treatments at the entitled ward.
Get higher limits for the insured receiving treatment for multiple primary cancers under the Cancer Drug Treatment Benefit[7] and Cancer Drug Services Benefit[13].
You can use MediSave to pay your premiums (up to the Additional Withdrawal Limits[14], excluding riders). Future premiums are unaffected by your claims history[15], whether you have made numerous claims or none at all.
Receive a one-time Critical Care Benefit[26,27] of up to $50,000 if the insured child requires an intensive care unit (ICU) or high dependency unit (HDU) stay of 4 days or more in one hospital admission, providing greater peace of mind.
Choose your preferred healthcare plan based on your financial and medical needs
Enhanced Preferred
Enhanced Advantage
Enhanced Basic
For a more detailed look at what you are covered for, you may view the full coverage table here.
Seek medical care through our panel of trusted medical professionals
Access to our panels16 of over 600 specialists across various specialties and sub-specialties in private practice island-wide, specially curated to meet your medical needs at quality clinical standards.
Supplement your Enhanced IncomeShield with Optima Care or Essential Care rider
For withdrawn riders (Deluxe Care Rider, Classic Care Rider, Plus Rider, Assist Rider, Daily Cash Rider and Child Illness Rider), read more here.
What our customers have said about us!
Your policy toolkit
Eligibility and payment frequency
To apply or upgrade to Enhanced IncomeShield, the last entry age is 75 (based on the insured's age next birthday).
To apply for Optima Care Rider or Essential Care Rider, the last entry age is 75 (based on the insured's age next birthday). The plan selected for the Optima Care Rider or Essential Care Rider must be the same as your Enhanced IncomeShield plan.
You need to make payment every year.
View full premium table for Main Plan
View full premium table for Optima Care Rider
View full premium table for Essential Care Rider
You may refer to MOH’s website for a comparison of Integrated Shield Plans (IPs) across all insurers, including the estimated premiums you have to pay for an IP over your lifetime.
Learn more about the drivers of premium here.
Brochures
Your queries answered.
Optima Care Rider is a rider attached that covers the co-insurance part of your Enhanced IncomeShield plans.
Optima Care Rider is not available to Enhanced C policyholders. Should you have further queries, we would be most happy to assist you via your preferred mode of contact at income.com.sg/contact-us.
While this rider is in force, there is no co-insurance due under your policy. However, you will have to make a co-payment for each claim.
The benefits are as shown in the table.
|
Benefits |
Optima Care Rider | |||
| Panel1 | Extended Panel2 | Others | ||
| Cover co-insurance | Yes (benefit limits apply) | |||
| Co-payment of the benefits due under your policy | 5% | 8% | 8% | |
| Co-payment limit (each policy year) | Up to $6,000 limit | No limit | ||
| Cancer Drug Treatment Benefit Limit | ||||
| Treatment on the CDL3 (each month) |
One Primary Cancer:
Multiple Primary Cancers4:
|
|||
| Non-CDL treatment5 (each month) |
One Primary Cancer:
Multiple Primary Cancers4:
|
|||
| Co-payment for Cancer Drug Treatment and Cancer Drug Services (CDS) | ||||
| Treatment on the CDL | Co-payment of the benefits due under your policy | 5% | ||
| Co-payment limit (each policy year) | Up to $6,000 limit | No limit | ||
| Non-CDL treatment | Co-payment of the benefits due under your policy | 10% | ||
| Co-payment limit (each policy year) | No limit | |||
| CDS | Co-payment of the benefits due under your policy | 5% | ||
| Co-payment limit (each policy year) | Up to $6,000 limit | No limit | ||
| Cell, Tissue and Gene Therapy Benefit limit | ||||
| Treatment not on MOH’s CTGTP list (one treatment per indication per lifetime) | EP: $150,000
EA: $150,000
|
|||
| Co-payment for Cell, Tissue and Gene Therapy Benefit | ||||
|
Treatment not on MOH’s CTGTP list (one treatment per indication per lifetime) |
Co-payment of the benefits due under your policy | 10% | ||
| Co-payment limit (each policy year) | No limit | |||
| Other benefits | ||||
|
Pre-hospitalisation benefit (before admission) |
EP:
EA:
EB:
|
Not applicable | ||
|
Post-hospitalisation benefit (after discharge) |
EP:
EA:
EB:
|
EP:
Up to 80 additional days EA:
EB:
|
||
| Extra Bed benefit | Receive up to $80 each day (up to a maximum of 10 days each hospital stay) for the cost of an extra bed for you to sleep over if your insured child gets warded. We will only pay for the stay of one parent or guardian.
|
|||
| The benefits below are only payable for insured up to age 18 (next birthday) | ||||
| Autism Testing Benefit (once per lifetime) | EP: $1,000
EA: $500 EB: Not applicable |
|||
| Autism Testing Benefit | Co-payment of the benefits due under your policy | 10% | ||
| Co-payment limit (each policy year)
|
No limit | |||
| Critical Care Benefit (once per lifetime) | EP: $50,000
EA: $30,000 EB: Not applicable |
|||
| Critical Care Benefit | Co-payment of the benefits due under your policy | Not applicable | ||
| Co-payment limit (each policy year) | ||||
1Panel or preferred partner means a:
- registered medical practitioner;
- specialist;
- hospital;
- or medical institution;
approved by us. The lists of approved panels and preferred partners, which we may update from time to time, can be found at www.income.com.sg/specialist-panel. Our list of approved panels also includes all restructured hospitals, community hospitals and voluntary welfare organisations (VWO) dialysis centres.
2Extended panel means a registered medical practitioner or specialist approved by us to provide cover for the benefits under this rider. The registered medical practitioner or specialist must not also be on our lists of approved panels or preferred partners and must meet other criteria, including being on another Integrated Shield Plan provider’s panel list. The list of our approved extended panel can be found at income.com.sg/specialist-panel. We may update this list from time to time.
3Cancer Drug List (CDL) means the list of clinically proven and more cost-effective cancer drug treatments on the MOH website (go.gov.sg/moh-cancerdruglist). MOH may update the CDL from time to time.
4The term ‘multiple primary cancers’ is defined as two or more cancers arising from different sites and are of a different histology or morphology group. An application form for higher claim limits for the insured receiving treatment for multiple primary cancers is to be sent to Income Insurance and MOH by their registered medical practitioner for assessment of the Integrated Shield Plan and MediShield Life Plan coverage, respectively.
5For outpatient cancer drug treatments not on the CDL, Income Insurance covers only treatments with drug classes A to E (according to LIA’s Non-CDL Classification Framework). Refer to lia.org.sg/media/3553/non-cdl-classification-framework.pdf for more details. LIA may update the list from time to time.
If the treatment is provided by our panel1 or extended panel2, the co-payment limit per policy year is up to $6,000. Once the total accumulated co-payments exceed the co-payment limit of $6,000 for each policy year, no further co-payment shall be payable by you for the insured’s treatment provided by our panel or extended panel for the remainder of the same policy year.
If you are claiming for pre-hospitalisation treatment, post-hospitalisation treatment or special benefits (if covered), we will apply the co-payment limit only if the treatment during the insured’s stay in hospital is provided by our panel1 or extended panel2. We will apply the same co-payment percentage of the inpatient hospital treatment to the pre-hospitalisation treatment and post-hospitalisation treatment.
If you are claiming for consultation fees, medicines, examinations or tests for the main outpatient hospital treatment that is covered under your policy, we will apply the co-payment limit only if the main outpatient hospital treatment is provided by our panel1 or extended panel2. We will apply the same co-payment percentage for these consultation fees, medicines, examinations or tests as the main outpatient hospital treatment.
If you are making a claim under your policy for your stay in hospital that is a result of being admitted from the emergency department of the same hospital in the same visit, we will treat your claim as a treatment provided by our panel1.
For each claim that meets the limits on special benefits (if they apply) or the limit for each policy year of your policy, the co-payment for that claim will not count towards the co-payment limit of $6,000 for each policy year.
When the insured is under the care of more than one registered medical practitioner or specialist for their stay in hospital or the main outpatient hospital treatment under your policy, we will apply the co-payment limit as long as the main treating registered medical practitioner or specialist (shown in the hospital records as the principal doctor) is part of our panel1 or extended panel2.
For each stay in hospital of 12 months or less, where the treatment is provided by our panel1 or extended panel2, you must pay the co-payment (up to a maximum of $6,000) for one policy year (even if the stay in hospital runs into the next policy year). If the stay in hospital is for a continuous period of more than 12 months but less than 24 months, you must also pay up to the maximum co-payment for the next policy year. And, for each further period of 12 months or less that the stay in hospital extends for, you must pay the co-payment for one extra policy year.
1Panel or preferred partner means a:
- registered medical practitioner;
- specialist;
- hospital;
- or medical institution;
approved by us. The lists of approved panels and preferred partners, which we may update from time to time, can be found at income.com.sg/specialist-panel. Our list of approved panels also includes all restructured hospitals, community hospitals and voluntary welfare organisations (VWO) dialysis centres.
2Extended panel means a registered medical practitioner or specialist approved by us to provide cover for the benefits under this rider. The registered medical practitioner or specialist must not also be on our lists of approved panels or preferred partners and must meet other criteria, including being on another Integrated Shield Plan provider’s panel list. The list of our approved extended panel can be found at income.com.sg/specialist-panel. We may update this list from time to time.
This benefit is only applicable if your plan is either the Enhanced IncomeShield Preferred Plan or the Enhanced IncomeShield Advantage Plan.
This benefit applies on top of the pre-hospitalisation treatment benefit and post-hospitalisation treatment benefit covered under your Enhanced IncomeShield Preferred Plan or Enhanced IncomeShield Advantage Plan (where applicable).
| Types of treatment | Co-payment |
| Treatment on the CDL3 provided by our panel1 or extended panel2 | 5% co-payment and co-payment limit of $6,000 each policy year |
| Treatment on the CDL3 not provided by our panel1 or extended panel2 | 5% co-payment and no co-payment limit |
| Non-CDL treatment | 10% co-payment and no co-payment limit |
| Cancer Drug Services provided by our panel1 or extended panel2 | 5% co-payment and co-payment limit of $6,000 each policy year |
| Cancer Drug Services not provided by our panel1 or extended panel2 | 5% co-payment and no co-payment limit |
1Panel or preferred partner means a:
- registered medical practitioner;
- specialist;
- hospital;
- or medical institution;
approved by us. The lists of approved panels and preferred partners, which we may update from time to time, can be found at income.com.sg/specialist-panel. Our list of approved panels also includes all restructured hospitals, community hospitals and voluntary welfare organisations (VWO) dialysis centres.
2Extended panel means a registered medical practitioner or specialist approved by us to provide cover for the benefits under this rider. The registered medical practitioner or specialist must not also be on our lists of approved panels or preferred partners and must meet other criteria, including being on another Integrated Shield Plan provider’s panel list. The list of our approved extended panel can be found at income.com.sg/specialist-panel. We may update this list from time to time.
3Cancer Drug List (CDL) means the list of clinically proven and more cost-effective cancer drug treatments on the MOH website (go.gov.sg/moh-cancerdruglist). MOH may update the CDL from time to time.
If the treatment is not on MOH’s CTGTP list but is approved by the Health Sciences Authority (HSA), you will have to make a co-payment of 10% of the benefits due under this rider. There will not be a co-payment limit.
You may make a claim under this benefit as long as you have not fully used the benefit payable up to the applicable benefit limit.
The insured must be age 18 or younger during the stay in hospital and the insured’s parent or guardian stayed and shared in the same room. We will only pay for the stay of one parent or guardian. We will pay up to 10 days for each stay in hospital. If the insured is in the hospital for only part of a day, we will pay half of this benefit for that day. You do not need to pay the co-payment if we pay this benefit.
The insured must be age 18 or younger and must have undergone an autism test. There must be a referral from a paediatrician for the autism test. You will have to make a co-payment of 10% of the benefits due under this rider.
The insured must be age 18 or younger and have stayed in an intensive care unit (ICU) or high dependency unit (HDU) for a total of 4 days or more in one hospital admission. This benefit is only payable once in the lifetime of your policy. You do not need to pay the co-payment if we pay this benefit.
This benefit is not payable for the following:
- the insured suffered symptoms of, had investigations for, or was diagnosed with illness any time before or within 90 days from the start date of this rider (except for accidents).
- claims for overseas treatment, including emergency overseas treatment.
Essential Care Rider is a rider attached that covers the co-insurance part of your Enhanced IncomeShield plans.
Essential Care Rider is not available to Enhanced C policyholders. Should you have further queries, we would be most happy to assist you via your preferred mode of contact at income.com.sg/contact-us.
While this rider is in force, there is no co-insurance due under your policy. However, you will have to make a co-payment for each claim.
The benefits are as shown in the table.
|
Benefits |
Essential Care Rider | |||
| Panel1 | Extended Panel2 | Others | ||
| Cover co-insurance | Yes (benefit limits apply) | |||
| Co-payment of the benefits due under your policy | 7% | 10% | 10% | |
| Co-payment limit (each policy year) | Up to $6,000 limit | No limit | ||
| Cancer Drug Treatment Benefit Limit | ||||
| Treatment on the CDL3 (each month) |
One Primary Cancer:
Multiple Primary Cancers4:
|
|||
| Non-CDL treatment5 (each month) |
One Primary Cancer:
Multiple Primary Cancers4:
|
|||
| Co-payment for Cancer Drug Treatment and Cancer Drug Services (CDS) | ||||
| Treatment on the CDL | Co-payment of the benefits due under your policy | 10% | ||
| Co-payment limit (each policy year) | Up to $6,000 limit | No limit | ||
| Non-CDL treatment | Co-payment of the benefits due under your policy | 20% | ||
| Co-payment limit (each policy year) | No limit | |||
| CDS | Co-payment of the benefits due under your policy | 10% | ||
| Co-payment limit (each policy year) | Up to $6,000 limit | No limit | ||
| Cell, Tissue and Gene Therapy Benefit limit | ||||
| Treatment not on MOH’s CTGTP list (one treatment per indication per lifetime) | EP: $150,000
EA: $150,000
|
|||
| Co-payment for Cell, Tissue and Gene Therapy Benefit | ||||
|
Treatment not on MOH’s CTGTP list (one treatment per indication per lifetime) |
Co-payment of the benefits due under your policy | 20% | ||
| Co-payment limit (each policy year) | No limit | |||
| Other benefits | Extra Bed benefit | Receive up to $80 each day (up to a maximum of 10 days each hospital stay) for the cost of an extra bed for you to sleep over if your insured child gets warded. We will only pay for the stay of one parent or guardian.
|
||
1Panel or preferred partner means a:
- registered medical practitioner;
- specialist;
- hospital;
- or medical institution;
approved by us. The lists of approved panels and preferred partners, which we may update from time to time, can be found at www.income.com.sg/specialist-panel. Our list of approved panels also includes all restructured hospitals, community hospitals and voluntary welfare organisations (VWO) dialysis centres.
2Extended panel means a registered medical practitioner or specialist approved by us to provide cover for the benefits under this rider. The registered medical practitioner or specialist must not also be on our lists of approved panels or preferred partners and must meet other criteria, including being on another Integrated Shield Plan provider’s panel list. The list of our approved extended panel can be found at income.com.sg/specialist-panel. We may update this list from time to time.
3Cancer Drug List (CDL) means the list of clinically proven and more cost-effective cancer drug treatments on the MOH website (go.gov.sg/moh-cancerdruglist). MOH may update the CDL from time to time.
4The term ‘multiple primary cancers’ is defined as two or more cancers arising from different sites and are of a different histology or morphology group. An application form for higher claim limits for the insured receiving treatment for multiple primary cancers is to be sent to Income Insurance and MOH by their registered medical practitioner for assessment of the Integrated Shield Plan and MediShield Life Plan coverage, respectively.
5For outpatient cancer drug treatments not on the CDL, Income Insurance covers only treatments with drug classes A to E (according to LIA’s Non-CDL Classification Framework). Refer to lia.org.sg/media/3553/non-cdl-classification-framework.pdf for more details. LIA may update the list from time to time.
If the treatment is provided by our panel1 or extended panel2, the co-payment limit per policy year is up to $6,000. Once the total accumulated co-payments exceed the co-payment limit of $6,000 for each policy year, no further co-payment shall be payable by you for the insured’s treatment provided by our panel or extended panel for the remainder of the same policy year.
If you are claiming for pre-hospitalisation treatment, post-hospitalisation treatment or special benefits (if covered), we will apply the co-payment limit only if the treatment during the insured’s stay in hospital is provided by our panel1 or extended panel2. We will apply the same co-payment percentage of the inpatient hospital treatment to the pre-hospitalisation treatment and post-hospitalisation treatment.
If you are claiming for consultation fees, medicines, examinations or tests for the main outpatient hospital treatment that is covered under your policy, we will apply the co-payment limit only if the main outpatient hospital treatment is provided by our panel1 or extended panel2. We will apply the same co-payment percentage for these consultation fees, medicines, examinations or tests as the main outpatient hospital treatment.
If you are making a claim under your policy for your stay in hospital that is a result of being admitted from the emergency department of the same hospital in the same visit, we will treat your claim as a treatment provided by our panel1.
For each claim that meets the limits on special benefits (if they apply) or the limit for each policy year of your policy, the co-payment for that claim will not count towards the co-payment limit of $6,000 for each policy year.
When the insured is under the care of more than one registered medical practitioner or specialist for their stay in hospital or the main outpatient hospital treatment under your policy, we will apply the co-payment limit as long as the main treating registered medical practitioner or specialist (shown in the hospital records as the principal doctor) is part of our panel1 or extended panel2.
For each stay in hospital of 12 months or less, where the treatment is provided by our panel1 or extended panel2, you must pay the co-payment (up to a maximum of $6,000) for one policy year (even if the stay in hospital runs into the next policy year). If the stay in hospital is for a continuous period of more than 12 months but less than 24 months, you must also pay up to the maximum co-payment for the next policy year. And, for each further period of 12 months or less that the stay in hospital extends for, you must pay the co-payment for one extra policy year.
1Panel or preferred partner means a:
- registered medical practitioner;
- specialist;
- hospital;
- or medical institution;
approved by us. The lists of approved panels and preferred partners, which we may update from time to time, can be found at income.com.sg/specialist-panel. Our list of approved panels also includes all restructured hospitals, community hospitals and voluntary welfare organisations (VWO) dialysis centres.
2Extended panel means a registered medical practitioner or specialist approved by us to provide cover for the benefits under this rider. The registered medical practitioner or specialist must not also be on our lists of approved panels or preferred partners and must meet other criteria, including being on another Integrated Shield Plan provider’s panel list. The list of our approved extended panel can be found at income.com.sg/specialist-panel. We may update this list from time to time.
| Types of treatment | Co-payment |
| Treatment on the CDL3 provided by our panel1 or extended panel2 | 10% co-payment and co-payment limit of $6,000 each policy year |
| Treatment on the CDL3 not provided by our panel1 or extended panel2 | 10% co-payment and no co-payment limit |
| Non-CDL treatment | 20% co-payment and no co-payment limit |
| Cancer Drug Services provided by our panel1 or extended panel2 | 10% co-payment and co-payment limit of $6,000 each policy year |
| Cancer Drug Services not provided by our panel1 or extended panel2 | 10% co-payment and no co-payment limit |
1Panel or preferred partner means a:
- registered medical practitioner;
- specialist;
- hospital;
- or medical institution;
approved by us. The lists of approved panels and preferred partners, which we may update from time to time, can be found at income.com.sg/specialist-panel. Our list of approved panels also includes all restructured hospitals, community hospitals and voluntary welfare organisations (VWO) dialysis centres.
2Extended panel means a registered medical practitioner or specialist approved by us to provide cover for the benefits under this rider. The registered medical practitioner or specialist must not also be on our lists of approved panels or preferred partners and must meet other criteria, including being on another Integrated Shield Plan provider’s panel list. The list of our approved extended panel can be found at income.com.sg/specialist-panel. We may update this list from time to time.
3Cancer Drug List (CDL) means the list of clinically proven and more cost-effective cancer drug treatments on the MOH website (go.gov.sg/moh-cancerdruglist). MOH may update the CDL from time to time.
If the treatment is not on MOH’s CTGTP list but is approved by the Health Sciences Authority (HSA), you will have to make a co-payment of 20% of the benefits due under this rider. There will not be a co-payment limit.
You may make a claim under this benefit as long as you have not fully used the benefit payable up to the applicable benefit limit.
The insured must be age 18 or younger during the stay in hospital and the insured’s parent or guardian stayed and shared in the same room. We will only pay for the stay of one parent or guardian. We will pay up to 10 days for each stay in hospital. If the insured is in the hospital for only part of a day, we will pay half of this benefit for that day. You do not need to pay the co-payment if we pay this benefit.
An Integrated Shield Plan (IP) consists of two parts – the MediShield Life portion which is managed by the Central Provident Fund (CPF) Board and an additional private insurance coverage portion offered by a private insurer.
The MediShield Life portion is designed for Class B2/C wards stays in restructured hospitals. The additional insurance coverage offered by the private insurer will increase your level of protection beyond medical care provided at Class B2/C wards in restructured hospitals.
Enhanced IncomeShield are IPs offered by Income Insurance Limited (Income Insurance).
The MediShield Life portion is designed to cover treatment in Class B2/C wards in restructured hospitals and pays only up to MediShield Life benefit limits, when you stay in higher class wards in restructured hospitals or private hospitals. With lower or no government subsidies, treatments at higher class wards in restructured hospitals or private hospitals are more expensive.
Enhanced IncomeShield helps to provide Singapore Citizens and Permanent Residents who wish to stay in higher ward classes with additional coverage so that policyholders can be more adequately protected.
Enhanced IncomeShield also covers you for certain benefits that are not included under MediShield Life. This includes coverage for pre- and post-hospitalisation expenses, emergency overseas treatment, and the option to purchase riders to cover deductibles and co-insurance. With these benefits, Enhanced IncomeShield takes care of your hospital and surgical expenses and provides you with peace of mind while you recuperate. With higher benefits, Enhanced IncomeShield premiums are also higher than MediShield Life premiums.
We encourage you to decide on a plan that meets your needs, taking into consideration your preferred ward class and level of benefits, and affordability of premiums over the long-term.
There is no duplicate coverage between MediShield Life and Enhanced IncomeShield.
Policyholders covered under Enhanced IncomeShield will enjoy the combined benefits of MediShield Life which provides hospitalisation coverage targeted at Class B2/C wards and the additional private insurance coverage targeted at higher class wards in restructured or even private hospitals depending on your plan.
Your Enhanced IncomeShield premium is made up of the MediShield Life premium and an additional private insurance coverage premium. Hence, you are not paying double premiums.
Enhanced IncomeShield policyholders will receive the applicable MediShield Life subsidies for the MediShield Life portion.
MediShield Life is able to cover pre-existing conditions because the cost of providing such coverage is shared among those with pre-existing conditions, the community and the government, which bears the bulk of the costs.
Unlike MediShield Life, private insurers are unable to provide cover for pre-existing conditions. Hence, these pre-existing conditions will continue to be excluded from the additional private insurance coverage portion under your Enhanced IncomeShield.
Riders are not part of Integrated Shield Plans (IPs), as they are not approved by Ministry of Health (MOH) for MediSave use.
Riders are complementary products introduced by private insurers to cover the co-insurance and deductible portions of your bill when you make a claim under your Integrated Shield Plan (IP). Some riders also provide additional benefits when you are hospitalised. Please refer to the respective policy contract for more information.
As Riders are not MediSave-approved plans, policyholders will need to pay for them separately by cash.
With the launch of MediShield Life, there will be two parts to MediSave’s use for IP premiums.
The first part is for MediShield Life premiums which can be fully payable by MediSave.
The second part is called the Additional Withdrawal Limit (AWLs), which is the maximum MediSave limit that you can use for your Enhanced IncomeShield’s additional private insurance coverage premiums.
If your additional private insurance coverage premium costs more than the AWL, you will have to pay the balance in cash. You can refer to the Cash Outlay indicated in your payment notice letter. With the new AWLs, Singaporeans will be able to use the same amount or more of their MediSave to pay the additional private insurance coverage component of their IP premiums than before. This is provided that there is no change in plans or age bands.
Deductible means the part of the benefit you are claiming that the insured must pay before we will pay any benefit. The deductible is shown in the schedule of benefits. Co-insurance means the amount that you need to pay after the deductible. The co-insurance percentages for the benefits are shown in the schedule of benefits. Co-insurance applies to all claims made under your policy except for final expenses benefit.
After you have been accepted, any change to your health status does not affect your current insurance coverage.
You can access our health coverage tool here to find out if your treatment is covered under your plan and get helpful information you need to file your claims. All claims submitted are subjected to review in accordance with the terms and conditions of the policies.
No, you can only be insured under one Integrated Shield Plan at any point in time. Your current Integrated Shield Plan will be automatically terminated upon commencement of a new Integrated Shield Plan.
Income Insurance will apply its own guidelines on the assessment of risks. If you have any additional information about your health, you may give this to us for a review of our earlier decision.
Yes, you can submit your medical reports to us for our review. If the medical reports submitted do not have sufficient information, we may request for more information. We reserve the right to maintain our initial decision if the improvement of the medical condition does not meet our underwriting guidelines.
For existing IncomeShield policyholders, you can choose to upgrade your plan to enjoy better benefit by submitting an upgrade request via My Income customer portal or you can speak to your advisor.
You will need to meet the entry requirements (e.g. maximum entry age) of the plan you wish to upgrade to. Any upgrade of plans will require underwriting.
No, you will continue to enjoy cover up to the benefit limits of your previous plan for these medical conditions. For your upgraded plan, you will be covered for any other medical conditions that you are not excluded from.
No, upon approval of your upgrade application, we will issue you a new policy contract. The change will take effect on the start date indicated on your policy contract. To upgrade to Enhanced IncomeShield plans, you need to be 75 years old and below (age next birthday).
Upon a request to upgrade your plan, the current policy will be terminated and a new set of policy document will be issued to you. Any unused premiums from the terminated policy will be refunded to you.
We are using the same policy number for your new plan as it is essentially a conversion or upgrade of plan. This will make it easier for you to remember your policy number.
If you wish to upgrade to a higher plan after your first upgrade, you can do so after 40 days from the start date of your upgraded plan.
The refund of your pro-rated premium for your previous plan can only be processed after CPF Board confirms the activation of your upgraded plan. Furthermore, refunds are processed in batches. Therefore, the refund for your previous plan and the premium deduction for your upgraded plan may not coincide.
Each insured person is issued an individual insurance policy. Therefore, each upgrade is processed independently and may result in a time difference when receiving your policy contracts.
Yes, you can. However, you should note that re-application will be subject to Income Insurance’s underwriting and acceptance.
You are only able to purchase either Optima Care Rider or Essential Care Rider.
You may get in touch with us through your preferred mode of contact at income.com.sg/contact-us or visit any of our branches to find out more if you are upgrading or adding Rider to Enhanced IncomeShield plans (Enhanced Preferred/Advantage/Basic).
Note
- You are not able to apply for an upgrade or add a new Rider to Enhanced IncomeShield Enhanced C plan and IncomeShield plans (Plan P/Plan A/Plan B/Plan C) as these plans are withdrawn. You are not able to apply for an upgrade or add a new Rider to IncomeShield Standard Plan as there are no rider options for IncomeShield Standard Plan. You may upgrade to our Enhanced IncomeShield plan (Enhanced Preferred/Advantage/Basic) and upgrade or add Rider to these plans.
- If the start date of the new Rider is not aligned with the Enhanced IncomeShield’s policy renewal date, a pro-rated premium will be charged for the new Rider. Upon the renewal of the Enhanced IncomeShield policy, the Rider renewal dates will be aligned with that of the Enhanced IncomeShield policy.
All the exclusions under the Enhanced IncomeShield/IncomeShield/IncomeShield Standard Plan will apply to the Riders. Additional exclusions under the Riders will be specified under the Rider contract.
If you are a Singapore Citizen or Permanent Resident, even though you have terminated your Enhanced IncomeShield/IncomeShield/ IncomeShield Standard Plan, you will continue to be covered under MediShield Life.
We would like to highlight that by terminating your Enhanced IncomeShield/IncomeShield/IncomeShield Standard Plan, you will need to re-apply if you wish to be covered in the future. The acceptance of your new application will be subject to Income Insurance’s underwriting and acceptance. Before you terminate the cover, we hope that you will reconsider your decision as it is important for you to have medical insurance coverage to help defray part of the large medical bills in the event of a serious illness or prolonged hospitalisation.
Your re-application for Enhanced IncomeShield/IncomeShield/IncomeShield Standard Plan will be subject to Income Insurance’s underwriting and acceptance. Depending on the underwriting assessment, your application may be:
- Accepted at standard terms
- Accepted with exclusions on any pre-existing medical conditions
- Postponed or Declined
Anyone who pays for, or is insured under Enhanced IncomeShield is not eligible for Additional Premium Support (APS) from the Government. ^
If you are currently receiving APS to pay for your MediShield Life and/or CareShield Life premiums, and you choose to be insured under Enhanced IncomeShield, you will stop receiving APS. This applies even if you are not the person paying for Enhanced IncomeShield. In addition, if you choose to be insured under Enhanced IncomeShield, the person paying for Enhanced IncomeShield will stop receiving APS, if he or she is currently receiving APS.
^ APS is for families who need assistance with MediShield Life and/or CareShield Life premiums, even after receiving premium subsidies and making use of MediSave to pay for these premiums.
You may submit your claims via My Income customer portal. For more information on our claim process and other channels to submit your claims, find out more here.
Understand the details
#Based on a survey by Nielsen IQ between January 2023 to December 2025, with 11,040 health insurance policyholders between 21 and 65 years old, Income Insurance ranked first at 33% as a health insurance company that can be trusted in good and bad times.
^Applicable to selected plan types and benefits.
*We offer 15% off (“Welcome Discount”) on your first-year premium with the purchase of Enhanced IncomeShield Preferred, Advantage or Basic Plan (each a “Qualifying Policy”) and/or Optima Care Rider or Essential Care Rider (each a “Rider”). The Welcome Discount is only applicable if no additional exclusion or premium loading is applied to the Qualifying Policy and applicable Riders upon policy issuance. The Welcome Discount is only applicable to a Rider if the Rider is taken up together with the Qualifying Policy. The Welcome Discount does not apply to the premium for the MediShield Life portion. Welcome Discount terms and conditions apply. Please refer to income.com.sg/integrated-shield-plan/welcome-discount-tnc.pdf for further details.
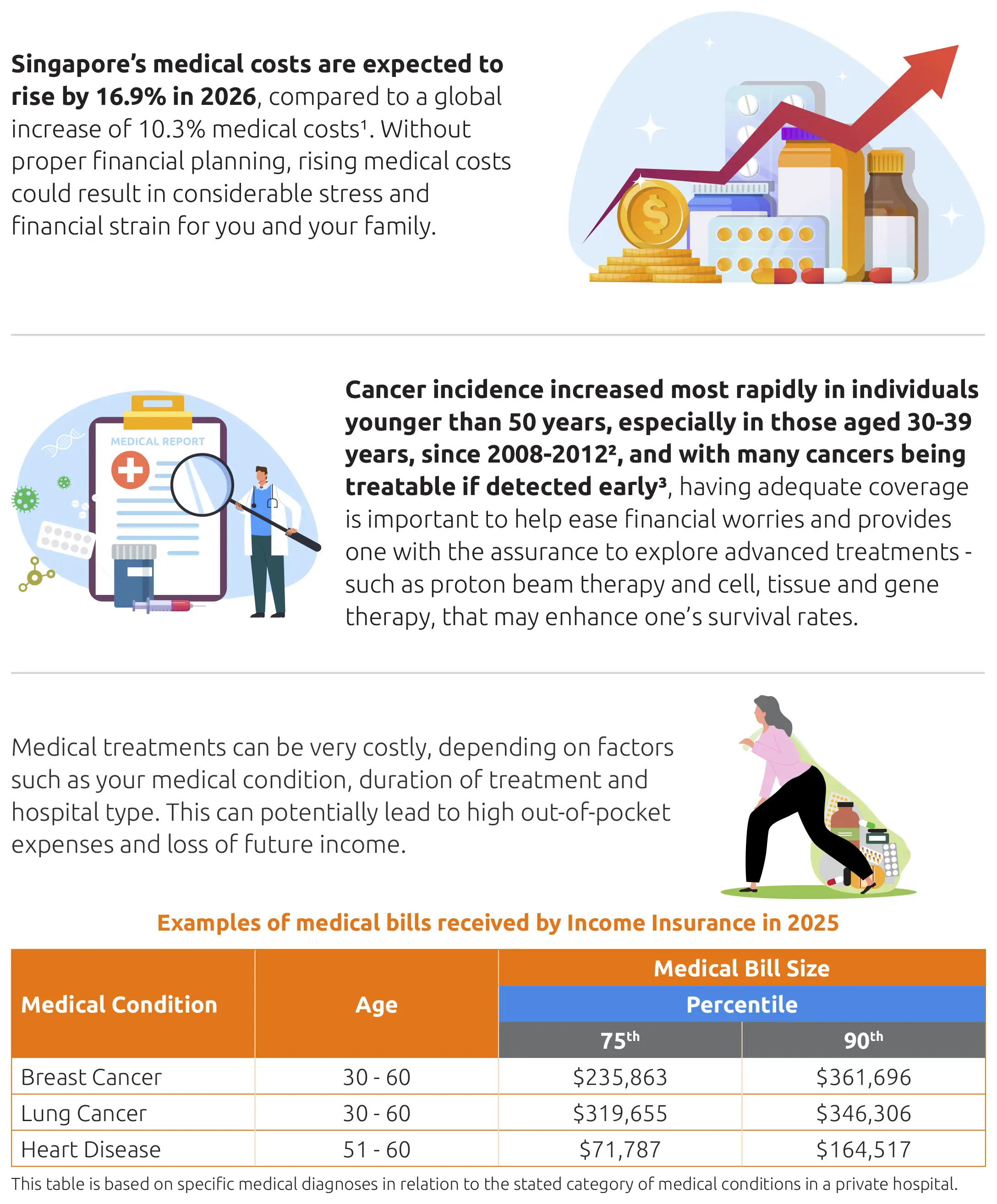
[1]Business Times, Singapore insurers brace for 2026 as medical inflation climbs and IP rules tighten.
[2]National Registry of Diseases Office, Singapore Cancer Registry Infographic 2022.
[3]National Registry of Diseases Office, Singapore Cancer Registry 50th Anniversary Monograph 1968-2017.
[4]Applicable to Enhanced Preferred Plan only.
[5]Subject to policy year limits and any benefit limits.
[6]Enhanced IncomeShield covers 5x MediShield Life (MSHL) Limit and 18x MSHL Limit for one primary cancer when you add an Optima Care or Essential Care rider to your Enhanced Preferred or Enhanced Advantage plan.
[7]This benefit covers the main outpatient hospital treatment received by the insured from a hospital or a licensed medical centre or clinic. For cancer drug treatment, only cancer drug treatments listed on the Cancer Drug List (CDL) and used according to the indications for the cancer drugs, as specified in the CDL on Ministry of Health (MOH) website (go.gov.sg/moh-cancerdruglist) will be covered. For each primary cancer, if the cancer drug treatment on the CDL involves more than one drug, we allow a particular drug to be removed from the treatment or replaced with another drug on the CDL that has the indication ‘for cancer treatment’, only if this is due to intolerance or contraindications (for example, allergic reactions). In such cases, the claim limit of the original cancer drug treatment on the CDL will apply.
For each primary cancer, if more than one cancer drug treatment is administered in a month, the following will apply.
- If any of the cancer drug treatments that are on the CDL has an indication that states ‘monotherapy’, only the treatments on the CDL that have the indication ‘for cancer treatment’ will be covered in that month.
- If none of the cancer drug treatments that are on the CDL has an indication that states ‘monotherapy’:
- if more than one of the cancer drug treatments administered in a month has an indication other than ‘for cancer treatment’, only cancer drug treatments that are on the CDL and have the indication ‘for cancer treatment’ will be covered in that month; and
- if one or none of the cancer drug treatments administered in a month has an indication other than ‘for cancer treatment’, all cancer drug treatments that are on the CDL will be covered in that month.
Cancer drug treatments not on the CDL will be considered as having an indication other than ‘for cancer treatment’.
For insured receiving treatment for one primary cancer, we will pay up to the highest limit among the covered cancer drug treatments on the CDL that are administered in that month.
The cancer drug treatment on the CDL benefit limit is based on a multiple of the MSHL Limit for the specific cancer drug treatment. For the latest MSHL Limit, refer to the CDL on MOH’s website under “MediShield Life Claim Limit per month” (go.gov.sg/moh-cancerdruglist). MOH may update this from time to time. The revised list will be applicable to the cancer drug treatment which occurred on and from the effective date of the revised list.
You do not have to pay a deductible for outpatient hospital treatment benefit.
[8]Applicable to Enhanced Preferred and Enhanced Advantage plans only.
[9]Cell, tissue and gene therapy benefit pays for cell, tissue and gene therapy provided to the insured which is on MOH’s Cell, Tissue and Gene Therapy Product (CTGTP) list as long as the following conditions are met.
- The cell, tissue and gene therapy is approved by MOH and Health Sciences Authority (HSA).
- The registered medical practitioner recommends in writing that the insured needs the cell, tissue and gene therapy for necessary medical treatment, according to the relevant guidelines from MOH.
- The cell, tissue and gene therapy is on MOH’s CTGTP list, and is provided to the insured according to the indications on the CTGTP list, as shown on MOH’s website (go.gov.sg/ctgtp-list). MOH may update this list from time to time. We will only cover the cell, tissue and gene therapies listed in the schedule of benefits.
We will not pay the cell, tissue and gene therapy benefit under any other benefit, regardless of whether the cell, tissue and gene therapy is provided as inpatient or outpatient hospital treatment.
[10]We will only cover the proton beam therapy if it is administered for an MOH-approved proton beam therapy indication (that is, MOH has approved the therapy for the insured’s condition) and the insured meets the eligibility criteria for proton beam therapy under MSHL. The proton beam therapy indications and the eligibility criteria are set out on MOH’s website (go.gov.sg/pbt-approved-indications). MOH may update these from time to time.
[11]Pre-hospitalisation and post-hospitalisation treatment are not covered for treatment given before or after inpatient psychiatric treatment, accident inpatient dental treatment or emergency overseas treatment. We do not cover pre-hospitalisation and post-hospitalisation treatment if, under the policy, we do not pay for the inpatient hospital treatment received during the stay in the hospital. Post-hospitalisation treatment, such as medication bought during a period of post-hospitalisation treatment but not used during that period, is not covered.
If the inpatient hospital treatment is provided by our panel and paid for under the Enhanced IncomeShield Preferred plan, we will cover the cost of medical treatment the insured received in the policy year for up to 180 days before the date they went into the hospital and up to 365 days after the date they left the hospital.
Please refer to the policy conditions for further details.
[12]We will reimburse you for the eligible hospitalisation cost you have incurred, subject to deductible, co-insurance, admission of ward class, benefit limits, and any other policy terms (including exclusions).
[13]For cancer drug services, it covers services that are part of any outpatient cancer drug treatment, such as consultations, scans, lab investigations, preparing and administering the cancer drug, supportive-care drugs and blood transfusions. It does not cover services provided before the insured is diagnosed with cancer or after the cancer drug treatment has ended.
The cancer drug services benefit limit is based on a multiple of the MSHL Limit for cancer drug services. For the latest MSHL Limit for cancer drug services, refer to “Cancer Drug Services” under the MSHL benefits on MOH’s website (go.gov.sg/mshlbenefits). MOH may update this from time to time. The revised limit will be applicable to the cancer drug services incurred within the policy year of the revised limit.
[14]The Additional Withdrawal Limit (AWL) is the maximum MediSave limit that you can use for your Enhanced IncomeShield’s additional private insurance coverage premiums. Please refer to moh.gov.sg/healthcare-schemes-subsidies/medishield-life for the latest AWL.
[15]The premiums of Enhanced IncomeShield are based on factors such as medical inflation and overall claims experience. There is no additional premium loading on individual policies that have made claim(s).
[16]Panel or preferred partner means a registered medical practitioner, specialist, hospital or medical institution approved by us. Our list of approved panels also includes all restructured hospitals, community hospitals and voluntary welfare organisations (VWO) dialysis centres.
Extended panel means a registered medical practitioner or specialist approved by us to provide cover for the benefits under this rider. The registered medical practitioner or specialist must not also be on our lists of approved panels or preferred partners and must meet other criteria, including being on another Integrated Shield Plan provider’s panel list.
The list of our approved panels, preferred partners, and extended panel can be found at income.com.sg/specialist-panel. We may update this list from time to time.
[17]Subject to precise terms, conditions and exclusions specified in the policy conditions for Enhanced IncomeShield and riders.
[18]For each outpatient cancer drug treatment claim under your policy (including this rider), you will have to make a co-payment of the benefits due under your policy as shown in the policy conditions. If the insured receives cancer drug treatment that is on the CDL and is provided by our panel or extended panel, the co-payment for that claim will count towards the co-payment limit of $6,000 in the policy conditions. To avoid doubt, we will not apply the co-payment limit for all non-CDL treatments, even if they are provided by our panel or extended panel. For each cancer drug services claim under your policy, you will have to make a co-payment of the benefits due under your policy as shown in the policy conditions. If the insured receives cancer drug services provided by our panel or extended panel, the co-payment for that claim will count towards the co-payment limit of $6,000 in the policy conditions.
[19]For outpatient cancer drug treatments not on the CDL, we cover only treatments with drug classes A to E (according to the Life Insurance Association, Singapore’s (LIA’s) Non-CDL Classification Framework). Refer to lia.org.sg/media/3553/non-cdl-classification-framework.pdf for more details. LIA may update the list from time to time.
[20]Cell, tissue and gene therapy benefit pays for all reasonable expenses for inpatient hospital treatment (including day surgery) and outpatient hospital treatment for cell, tissue and gene therapy (CTGTP) not on MOH’s CTGTP list (go.gov.sg/ctgtp-list) provided to the insured, up to the limits shown in the policy conditions, as long as the cell, tissue and gene therapy is approved by the HSA. When we pay the cell, tissue and gene therapy benefit under this rider, we add together all reasonable expenses for the cell, tissue and gene therapy treatment (including inpatient hospital treatment and outpatient hospital treatment), and pay up to the limits shown in the policy conditions.
You may make a claim under this benefit as long as you have not fully used the benefit payable up to the benefit limit in the policy conditions. We will pay the claim amount based on the following:
- If the claim amount after applying the co-payment is higher than the remaining benefit payable under this rider, we will pay up to the remaining benefit limit.
- If the claim amount after applying the co-payment is lower than the remaining benefit payable under this rider, you will have to make a co-payment of the benefits due under your policy as shown in the policy conditions and we will only pay the amount of your claim which is more than the co-payment.
[21]Pre-hospitalisation and post-hospitalisation benefit is only applicable if your plan is either the Enhanced IncomeShield Preferred plan or the Enhanced IncomeShield Advantage plan. This benefit applies on top of the pre-hospitalisation treatment benefit and post-hospitalisation treatment benefit covered under your Enhanced IncomeShield Preferred plan or Enhanced IncomeShield Advantage plan (where applicable), up to the limits shown in the policy conditions. Please refer to the policy conditions for further details.
[22]Pre-hospitalisation benefit covers up to 100 days before admission under the Enhanced Advantage plan and an additional up to 80 days before admission when you add an Optima Care rider and seek treatment provided by our panel.
[23]Post-hospitalisation benefit covers:
- up to 100 days after discharge under the Enhanced Preferred plan and an additional up to 80 days after discharge when you add an Optima Care rider and seek treatment not provided by our panel.
- up to 100 days after discharge under the Enhanced Advantage plan and an additional up to 80 days after discharge when you add an Optima Care rider and seek treatment provided by our panel.
[24]If, during the insured’s stay in hospital, their parent or guardian stays in the same room as the insured, we will reimburse up to $80 for each day the parent or guardian stays. We will only pay for the stay of one parent or guardian. This applies if the insured is a child aged 18 or younger during their stay in hospital. We will pay up to 10 days for each stay in hospital. If the insured is in hospital for only part of a day, we will pay half of this benefit for that day. Co-payment is not applicable for this benefit.
[25]Autism testing benefit is only payable for insured up to age 18 (next birthday) for the relevant plan. This benefit is payable if the insured undergoes an autism test, on a reimbursement basis, up to the limits for the relevant plan shown in the policy conditions. There must be a referral from a paediatrician for the autism test. This benefit is only payable once in the lifetime of your policy. You will have to make a 10% co-payment for each claim for this benefit due under your policy. Please refer to the policy conditions for further details on the co-payment limit.
[26]Critical care benefit is only payable for insured up to age 18 (next birthday) for the relevant plan. If the insured requires a stay in an intensive care unit (ICU) or high dependency unit (HDU) for a total of 4 days or more in one hospital admission, we will pay the benefit as shown in the policy conditions. The stay in the ICU or HDU must be confirmed as necessary medical treatment. We will not consider a stay in ICU or HDU as necessary medical treatment if the insured can be safely and adequately treated in any other facility. This benefit is not payable for the following:
- the insured suffered symptoms of, had investigations for, or was diagnosed with illness any time before or within 90 days from the start date of this rider (except for accidents).
- claims for overseas treatment, including emergency overseas treatment.
This benefit is only payable once in the lifetime of your policy. Co-payment is not applicable for this benefit.
[27]Applicable only when you add the Optima Care rider to your Enhanced Preferred or Enhanced Advantage plan.
There are certain conditions whereby the benefits under this plan will not be payable. You can refer to your policy conditions for the precise terms, conditions and exclusions of the plan. The policy conditions will be issued when your application is accepted.
Enhanced IncomeShield is available as a MediSave-approved Integrated Shield Plan for the insured who is a Singapore Citizen or a Singapore Permanent Resident. This applies as long as the insured meets the eligibility conditions under MediShield Life. If the insured is a foreigner who has an eligible valid pass with a foreign identification number (FIN), Enhanced IncomeShield is not available as an Integrated Shield Plan.
This is for general information only and does not constitute an offer, recommendation, solicitation, or advice to buy or sell any product(s). You can find the usual terms, conditions and exclusions of Enhanced IncomeShield plan here, Optima Care Rider here and Essential Care Rider here. All our products are developed to benefit our customers but not all may be suitable for your specific needs. If you are unsure if this product is suitable for you, we strongly encourage you to speak to a qualified insurance advisor. Otherwise, you may end up buying a product that does not meet your expectations or needs. As a result, you may not be able to afford the premiums or get the insurance protection you want. If you find that this policy is not suitable after purchasing it, you may terminate it within the free-look period and obtain a refund of the premiums paid.
This policy is protected under the Policy Owners’ Protection Scheme which is administered by the Singapore Deposit Insurance Corporation (SDIC). Coverage for your policy is automatic and no further action is required from you. For more information on the types of benefits that are covered under the scheme as well as the limits of coverage, where applicable, please contact Income Insurance or visit the GIA/LIA or SDIC websites (www.gia.org.sg or www.lia.org.sg or www.sdic.org.sg).
Protected by copyright and owned by Income Insurance Limited.
Information is correct as at 01 April 2026
Learn more about health insurance.

Delve into the world of insurance as we explore its significance in newlyweds' lives, from securing your love nest to safeguarding your health and finances.



